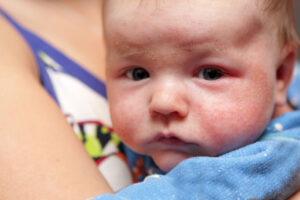
Eczema is an umbrella term for skin conditions that cause symptoms such as redness, blisters, scaling, oozing, crusting, pigmentation changes and thickened skin. The most common form of eczema is atopic eczema, which is allergy-related and is most common among children, although it can affect adults too. It can begin in infants as early as three months as a weepy red rash on the face and outer surfaces of arms and legs. It will be very itchy. In later childhood, it will manifest as a dry, scaly, itchy rash, often in the inner creases of the knees and elbows. There might also be rough patches with cracked skin on the palms and around the ears, and scaling of the scalp. The main focus of eczema treatment is on keeping skin moisturized.
Prevention
Infantile Eczema
Children can be accurately tested for allergies from four months of age. The risk of young children developing eczema is higher if their families suffer from severe eczema, asthma and nasal allergies. Preventative measures include both parents refraining from smoking during pregnancy and after birth, and the mother breast-feeding until the baby is six months old. While some allergy experts recommend avoiding common allergy-trigger foods such as eggs, cow’s milk, peanuts and fish while the mother is breast feeding, there is no convincing scientific evidence that this makes a significant difference.
About a third of infantile eczema cases are related to food allergies. In older children, food coloring and food additives can also aggravate eczema. Patients with eczema can also experience non-allergic skin irritation from Marmite; acidic citrus fruit such as limes and lemons; tomatoes; pineapples; berries; cheese; and chocolate.
Clothing
Avoid hot, humid and cold, dry weather as far as possible. Also try to avoid excessive sweating, wearing woolen or synthetic clothing close to the skin, and perfumed soaps. Cotton underwear, clothing and bed-linen are recommended.
Detergents
Avoid detergents as far as possible, and follow these tips:
- Install water softeners to the main household water supply if possible.
- Don’t use perfumed soaps, bubble bath, or household antiseptics in the bath.
- Chlorine can dry out the skin and irritate it, so avoid swimming pools if possible.
- Replace enzyme-enriched detergents with non-biological washing powders. Also add an extra rinse cycle on the washing machine.
At Night
When going to bed, cover as much skin as possible with non-allergenic, cotton clothing. Keep it lightweight though and ensure you don’t overdress or overheat children. Wearing light cotton gloves and having fingernails neatly clipped will reduce scratching during sleep. In more extreme cases, if you can’t stop your child scratching, elbow splints could be applied at night. Dust mite exposure can exacerbate eczema so measures to reduce their levels should be taken. Barrier bedding and microporous mattress covers will help.
Immunizations
Eczema normally starts at about three months old; the same time at which a baby has its first immunizations. This has led some parents to mistakenly see a causal link between the two, whereas it’s just a coincidence of timing.
Avoid Careers That Could Aggravate Your Condition
A career that would expose sufferers to irritant chemicals can be problematic. Young adults with eczema should probably avoid going into motor mechanics, nursing, hairdressing, catering, or the building industry. If exposure is unavoidable, wearing protective gloves with cotton inner-linings can help prevent irritant contact dermatitis.
Treatment
Keep Skin Moisturized
- Take Daily tepid baths, not showers, will hydrate your skin.
- Use mild, neutral soap, avoiding perfumed soap or deodorant.
- Apply moisturizers or lotions often (two to four times a day).
- Experiment with moisturizers and lotions to make sure you find one that least irritates your skin. Colloid baths can help moisturize your skin: Add 1 cup of cornstarch to your tepid bathwater, soak for 20 minutes, then air-dry before moisturizer liberally.
Reduce Itching & Scratching
- Avoid wool and other rough materials (try to stick to clothes made from cotton)
- Avoid laundry starch, fabric softeners and harsh detergents for clothes and bed sheets. Use mild detergent and always rinse well
- Stay away from hot and cold environments
- Avoid having long fingernails (adults should keep theirs trimmed, while infants and small children should also wear soft, cotton mittens)
- Stay away from dust, sprays, perfumes and animals
- Use the medicines you are prescribed
Steroid Creams
Steroid creams provide quick relief in the case of acute eczema, but should be used only for short periods, about five to seven days, to settle flare-ups. Long-term use can lead to a thinning of the skin. However, when diluted half-half with an emollient, they can be applied for longer periods and the treatment can be tapered off over a longer period. Some newer steroid creams have a better safety profile. Hydrocortisone 1% is mild and generally suitable for use on facial eczema, while eczema on the body normally requires stronger steroids such as mometasone, fluticasone and betamethasone. The most powerful topical steroid, clobetasol, should not be used anywhere else other than the feet and hands. Steroid injections and tablets are avoided in treating eczema due to their systemic side effects such as stunting growth, hormonal effects, and cataracts.
Wet Wraps
In extreme cases where little else works, our allergy specialist might recommend wet wraps. These can be particularly helpful for severe weepy eczema that is non-responsive to emollients and steroid creams. The wet cotton bandages are applied at night to help the skin retain moisture, to aid absorption of creams, and to prevent scratching. The first step is to apply the emollients and steroid creams your doctor has recommended to the eczematous areas. Next, the elasticated tubular dressings are soaked in tepid water and then cut to size so that fit over the affected areas. The wet wraps can be applied overnight to the limbs, trunk, neck and even face (with appropriate holes cut in them for ears, mouth, nose, etc).
Antibiotics
Eczema sufferers are more susceptible to skin infections such as viral bacterial and fungal infections, including ringworm and warts. Antibiotic creams (for example, Fucidin, Mupirocin) and, less frequently, antibiotic tablets (Flucloxacillin) are prescribed for Staphylococcus Aureus-infected eczema. This manifests as a sudden deterioration of eczema with redness of the skin, oozing and crusting. Adding a cap of Milton or Dettol to the bath can discourage Staphylococcal colonization of the skin, thus eliminating this potent trigger of unexplained outbreaks. Prolonged use of Fucidin can lead to bacterial resistance.
Antihistamines
Older sedating-type antihistamine syrup or tablets or syrup such as Promethazine or Chlorphenamine (Piriton) will reduce itching, and therefore damage to the skin, especially at during overnight. Antihistamine creams are not recommended though as they can sensitize the skin. Non-sedating anti-histamines like Desloratadine seem to be effective in reducing inflammation if used for periods of up to six months.
Other Therapies
Probiotic and prebiotic supplements
Research suggests that colonizing an infant’s immature bowel with “good” Acidophilus Probiotic microorganisms (for example, Lactobacillus rhamnosus GG and Bifidobacterium), while simultaneously giving Prebiotic supplementation (short-chain oligosaccharides), can delay or prevent atopic eczema developing. These supplements would be taken during pregnancy, while breastfeeding and in infancy.
Growing clinical evidence suggests that if you treat eczema aggressively in infancy it can reduce recurrences in later childhood. The newer topical steroid creams are very effective, minimally absorbed, and if you stick to the prescribed dosage, won’t lead to skin thinning.
Other Therapies
Evening Primrose and Omega 3 oil supplements have proved disappointing in treating eczema in clinical studies. Extracts of Chinese herbal teas appear to reduce inflammation, but they may cause liver damage. More encouraging initial results have been found using Tacrolimus (Protopic) and Pimecrolimus (Elidel), which are newer non-steroidal immune-modulating applications, especially in treating facial eczema, but sometimes cause initial redness and skin irritation.
Book your appointment at Novomed today!
To schedule a consultation with one of our expert dermatologists in Dubai, call us toll free at 8006686, fill out the booking form or click the live chat icon at the bottom of the screen.
































